Reports
Health
Wellness
Vitamin E is a group of 8 different nutrient compounds: 4 types of tocopherols and four types of tocotrienols. Both tocopherols and tocotrienols are types of vitamin E nutrients.
Image: Forms of Vitamin E
The most predominant form of vitamin E in the body is α-tocopherol. It comprises over 90% of the vitamin E found in the body. This form was first isolated from wheat germ oil. Interestingly, the “tokos” in α-tocopherol stands for “childbirth.”
Animal studies have revealed that a deficiency of α-tocopherol increases the risk of infertility. That’s why this nutrient is also known as anti-infertility vitamin or anti-sterility factor X.
Vitamin E is an essential nutrient, which means we need to obtain this nutrient through food sources.
Some foods rich in vitamin E are almonds, sunflower seeds, avocados, peanut butter, pine nuts, rainbow trout, and pumpkin.
Vitamin E is a potent antioxidant and protects our body from the damaging effects of free radicals.
Free radicals are unstable molecules that are harmful to the healthy cells in our bodies.
Vitamin E also has anti-aging properties.
Once vitamin E enters the body, it is absorbed by the intestines and stored in the adipose tissues, commonly known as body fat. On-demand, the adipose tissues are broken down to release vitamin E.
Here, it is important to know that the liver only acts on α-tocopherol and converts it into a form that is usable by the cells in the body. All other types of vitamin E are excreted out.
A healthy adult woman requires about 8 mg of vitamin E per day. In men and pregnant women, the requirement increases to 10 mg per day.
Vitamin E deficiency can result in a weakened immune system, muscle damage, vision loss, and nervous system-related disorders.
Many conditions like cystic fibrosis, short bowel syndrome, and chronic pancreatitis prevent effective absorption of fats, including the fat-soluble vitamin E. So, they can increase your risk for vitamin E deficiency.
Genetics is another important factor that contributes to vitamin E deficiency.
The TTPA gene is crucial for regulating vitamin E levels in the body. It contains instructions for the production of α-tocopherol transfer protein. This protein is responsible for the distribution of vitamin E obtained from the diet to all the cells and tissues of the body.
Any changes in this gene can affect the amount of the protein produced, and hence the vitamin E levels. People who have these changes are at a higher risk of vitamin E deficiency.
A simple genetic test can reveal your genetic status of vitamin E deficiency.
Most genetic tests provide your DNA information in the form of a text file called the raw DNA data. This data may seem like Greek and Latin to you.
At Xcode Life, can help you interpret this data. Upload your raw data and order a nutrition report.
Xcode Life then analyzes your raw data in detail to provide you with comprehensive nutrition analysis, including information on your vitamin E requirements.
Also Check Out: Gene Nutrition Report Walkthrough!
Folate (Vitamin B9) is also known as folic acid or folate. "Folic" is derived from the word "folium," meaning leaves, as in green leafy vegetables. Needless to say, leaves are one of the richest sources of vitamin B9.
The vitamin B9 we eat is absorbed in the jejunum region of the small intestine after going through minor structural changes.
In most cases, dietary sources of vitamin B9 are sufficient to meet this nutrient's requirement. Other than the leafy greens, some foods rich in vitamin B9 are beans, whole grains, seafood, peanuts, and sunflower seeds.
The Recommended Dietary Allowance or RDA for folate is 400 mcg/day for healthy adults. The RDA for lactating and pregnant women are 500 and 600 mcg/day, respectively.
Folate deficiency in pregnant women is one of the leading causes of neural tube defects, a birth abnormality, in babies.
Symptoms of vitamin B9 deficiency include extreme tiredness, pale skin, headaches, and heart palpitations.
Vitamin B9 needs to be converted into a form called tetrahydrofolate or THF to be effectively used by the body. The conversion of folic acid to THF is carried out by an enzyme called THF reductase.
This conversion is a very crucial step in the MTHFR cycle.
THF plays a very important role in converting a harmful amino acid called homocysteine to a safe and useful amino acid called methionine.
Image: Folate Cycle
The MTHFR gene is a well-known gene associated with folate deficiency. This gene helps the conversion of inactive vitamin B9 such as folate, or folic acid, to active B9, the THF.
30-60% of people have a change in this gene that ultimately leads to low vitamin B9 levels in the body.
Other genes like MTYL1 also influence your vitamin B9 levels.
Fortunately, vitamin B9 deficiency comes with a simple fix - increasing your dietary folate intake. In some cases, folate supplements may be advised.
A simple genetic test can reveal your genetic status of vitamin B9 deficiency.
Most genetic tests provide your DNA information in the form of a text file called the raw DNA data. This data may seem like Greek and Latin to you.
At Xcode Life, can help you interpret this data. Upload your raw data and order a nutrition report. Xcode Life then analyzes your raw data in detail to provide you with comprehensive nutrition analysis, including information on your vitamin B9 requirements.
Vitamin A is important for the overall development and maintenance of the body. Our body does not produce vitamin A on its own. It needs to be supplemented through diet; that's why it's called an essential vitamin.
The retina is the film screen, located at the very back of the eye. It contains two important cells that process the light entering our eyes.
The rod cells help us see in low light, while the cone cells help our color vision. The rod cells contain an important protein called rhodopsin, which moderates low light vision. A form of vitamin A called the retinal helps activate rhodopsin.
This is why a severe deficiency of vitamin A can cause night blindness.
Vitamin A is also crucial for maintaining skin integrity and forming new skin cells. Since vitamin A is an excellent antioxidant, including it in your diet every day can lower your risk for heart attack.
We all know that carrots are a good source of vitamin A. They are a rich source of a molecule called beta-carotene. Beta-carotene is a provitamin A. Provitamins are substances that are converted into active vitamins in the body.
Beta-carotene is what is responsible for the bright orange color of the carrot. All plants provide vitamin A in the form of beta-carotene, among other forms.
Vitamin A is present as retinol, a form of active vitamin A, in animal food sources. Now, the beta-carotene from plant sources must be converted to active vitamin A for it to be useful to the body.
Let’s see how that happens.
The structure of beta carotene resembles that of a dumbbell - two ring-like structures joined by a chain. This chain is cut in a particular way to give rise to two molecules of retinol, or active vitamin A. This cleavage happens in the liver.
Image: Cleavage of beta-carotene to retinol
Vitamin A in the body can be converted or interconverted into different formats. The retinol and retinal forms are interchangeable, while there’s only a one-way conversion from retinal to retinoic acid.
Image: Different forms of active vitamin A
The retinal form of vitamin A is absorbed by the intestinal villi along with fats. From there, it is transported to and stored in the liver. Whenever there's a requirement for vitamin A, retinal is released by the liver. It then binds to the specific retinol-binding protein, which serves as a carrier to transport it to various locations of the body.
The cleavage or the cutting of beta-carotene to form retinol is carried out by an enzyme called Beta Carotene Oxygenase or Monooxygenase. This enzyme is produced by the gene called BCMO1 or BCO1.
Every person has two copies of the BCMO1 gene. But, about 45 percent of the population carries at least one change or variation in the gene that reduces the enzyme activity. This results in a significantly impaired ability to convert beta-carotene into retinal.
Depending on which combination of variants someone has, beta-carotene conversion can be nearly 70 percent lower than its normal efficiency.
Vitamin A deficiency has serious health implications.
Knowing your BCMO1 gene status can help you gauge your genetic risk for vitamin A deficiency. This can be done through a genetic test.
Most genetic tests provide your DNA information in the form of a text file called the raw DNA data. This data may seem like Greek and Latin to you.
At Xcode Life, can help you interpret this data. All you have to do is upload your raw data and order a nutrition report. Xcode Life then analyzes your raw data in detail to provide you with comprehensive nutrition analysis, including information on your vitamin A requirements.
One of the most essential nutrients for the growth and development of the human body vitamin C. This is also known as ascorbic acid or ascorbate. This water-soluble vitamin cannot be made by the body and has to be obtained from the foods we eat.
Here are some of the significant functions of vitamin C:
Since vitamin C helps in producing collagen, it is a popular and widely used in the beauty and cosmetic industry.
Vitamin C deficiency is quite rare in developed countries. However, a very badly chosen diet and factors like excessive smoking or drug abuse can result in lowered vitamin C levels in the body and result in a variety of health problems.
Scurvy is a disease that has been known since the Egyptian and Greek times. It is caused by vitamin C deficiency and results in anemia, bleeding in gums, lowered Red Blood Cell count, and reduced healing rates. Scurvy can turn fatal if untreated.
The story of the discovery of vitamin C starts in the large vessels that carried Vasco da Gama and his sailors into the Indian and Pacific oceans in 1499. It is mentioned that Vasco da Gama lost two-thirds of his sailors to scurvy.
Similarly, Ferdinand Magellan, a Portuguese explorer lost 80% of his crew while crossing the Pacific ocean in 1520.
Scurvy remained one of the biggest reasons for sailor-deaths between the 1400s and 1700s.
James Lind was a surgeon in the UK Royal Navy and he started experimenting by giving two oranges and one lemon to a group of sailors and comparing their health with the others who did not receive the same.
He noticed that the sailors who received the oranges and lemon did not fall sick and were healthier than the rest of the crew members. He published his work on this experiment in 1753.
After that, sailing crew members were regularly provided with fresh lemon juice as a way to prevent them from falling sick. Many ports also had fruit trees growing abundantly for sailors and crew members to consume fruits when they anchored.
Vitamin C was finally identified in 1932 and is one of the first vitamins to be made on an industrial scale.
Vitamin C cannot be made by the body and you will have to get it directly from the foods you eat.
Vitamin C is absorbed by the body in the form of ascorbic acid (80-90%) and dehydroascorbic acid (10-20%).
Once ascorbic acid enters the intestine, it is transported by a particular transport protein called Sodium Vitamin C cotransporter (SVCT). Such cotransporter proteins help molecules move from one place to another inside the body.
Now, these ascorbic acid molecules are transported into the cells in the body using another set of transport proteins and are then used up.
Dehydroascorbic acid uses a set of glucose transporters and enters the cells in the body. These are then converted to ascorbic acid and then made use of in the cells.
Many people make a conscious effort to consume fruits and vegetables rich in vitamin C but do not enjoy the benefits. Do you know why?
Vitamin C is a gentle nutrient that gets destroyed very easily. Most of the common cooking methods kill vitamin C before it reaches your plate.
Vitamin C is destroyed by overexposure to light, heat, and air.
In a clinical study done in Nigeria in the year 2013, the vitamin C retaining capacity in peppers was studied. Peppers have 15.39 mg/25 ml vit C in raw form. The vitamin C quantity went down to 9.96 mg after just 15 minutes of cooking and to 5.43 mg after 30 minutes of cooking.
It is better to get your sources of vitamin C in raw form. However, if you want to cook, make sure you cook in low heat for minimal time and with as little water as you can. Vitamin C is water-soluble and hence when you boil food in lots of water and throw away the excess water, you are throwing out its nutrient value too.
The below-recommended values of vitamin C needed every day is put together by the Food and Nutrition Board (FNB).
Since Vitamin C is water-soluble, it does not get accumulated in the body and cause excess toxicity.
However, very large doses of vitamin C can result in symptoms like:
Most experts do mention that it is not easy to consume extremely high doses of vitamin C only through diet.
Only excessive consumption of supplements can cause the above effects.
Some of the top vitamin C deficiency signs to be aware of are:
Sodium Vitamin C cotransporter (SVCT) helps ascorbic acid reach the cells in the body. There are two genes SLC23A1 and SLC23A2 and their variations that create changes in vitamin C absorption levels.
Maintaining healthy ranges of vitamin C will keep you strong, active, and healthy.
Vitamin B6 (pyridoxine) is a water-soluble nutrient that cannot be made in the human body. You need to get B6 from the foods you eat or through nutritional supplements. This is a part of the B Vitamins group and is important for everyday functioning.
The functional (active) form of vitamin B6 is the Pyridoxal 5’ phosphate (PLP). PLP is a coenzyme (smaller molecules that help enzymes create a reaction in the body). The range of B6 in the blood is usually measured in terms of PLP levels.
Starting from the breaking down of carbohydrates, fats, and proteins to supporting brain health, PLP helps more than a hundred enzymes in the body to do their job right.
It is not surprising that B6 is considered a very important B vitamin. Here are some of the top benefits of maintaining right B6 levels in the blood.
It was only in the early 1900s that physicians and pathologists started working on the idea of inadequate nutrition leading to diseases. The idea that lack of nutrition can cause a variety of health conditions including death was intriguing to the great minds.
Scientists from the Merck Group of Pharma in the early 20th century played a great role in developing B Group vitamins on an industrial scale and this paved the way for the easy availability of B complex supplements to match growing needs in the community.
In 1934, Paul Gyorgy, an American biochemist and nutritionist was experimenting on rats, feeding them artificially created diets rich in already discovered B vitamins (B1 and B2).
He discovered that the rats developed skin allergies with the diet and when he fed them baker’s yeast, the condition disappeared.
He then extracted a particular compound from the yeast that helped cure skin allergies and named it vitamin B6. Later, Gyorgy and his fellow scientists also ended up extracting B6 from wheat germ and fish.
Paul Gyorgy is also known for the discovery of vitamin B2 and biotin and was later awarded the National Medal of Science for his efforts.
When you obtain vitamin B6 through natural sources, fortified foods, or supplements, it enters the stomach and then moves to the small intestine. Jejunum and ileum are two parts of the small intestine and B6 is absorbed here.
The process of absorption is known as passive diffusion (the molecules flow easily with no effort from a region of high concentration to a region of low concentration). The absorbed molecules are acted upon by a protein enzyme known as alkaline phosphatase. The vitamin is then converted to PLP in the jejunum’s inner layer.
PLP is passed on to the tissues and it helps the various enzymes in the body work effectively.
The remains of B6 after it gets converted to PLP are sent out through the urine. One of the major products sent out is 4-pyridoxic acid. In fact, up to 60% of ingested B6 is sent out as 4-pyridoxic acid.
People whose bodies do not absorb the right amounts of vitamin B6 have negligible 4-pyridoxic acid in the urine, and this is a clear indication of B6 deficiency.
Did you know that vitamin B6 is considered a complementary and alternative therapy for children diagnosed with autism?
From the time vitamin B6 was identified, there has been a group of scientists attempting to treat neurological disorders with these. The studies started in the 1950s for people with schizophrenia. They were treated with extra high doses of vitamin B6 and improvements were noted.
The Autism Research Institute (ARI) noted that about 49% of children who were treated with a combination of vitamin B6 and magnesium supplements showed improvements.
The relationship between vitamin B6 and autism is still being analyzed globally. We will hopefully find solid results very soon.
The Dietary recommended Intake (DRI) of vitamin B6 was set by the Food and Nutrition Board. The values depend on age and gender.
While mildly excess doses of vitamin B6 don’t cause any adverse effects, when you consume very high oral doses of B6 supplements for an extended period of time, it can result in certain sensory, skin, and gastric impairments.
Severely high doses of B6 can result in:
Here is a table that shows the daily tolerable upper limits for vitamin B6 in the body. Consuming more B6 than the levels mentioned here will cause the above side effects.
Usually, a person will not be deficient in just vitamin B6. He/she will have lower concentrations of other B complex vitamins too. Mild vitamin B6 deficiency does not show a lot of symptoms.
Severe deficiency or a prolonged period of deficiency will result in the following conditions.
In infants and younger children, lack of vitamin B6 is known to cause irritability and seizures.
There are two genes that cause people to require more vitamin B6 than the usual recommended ranges.
The ALPL gene plays a role in breaking down vitamin B6 from complex to simpler forms. It produces enzymes that help in clearance of B6.
A particular variant (type) of the gene can cause 12-18% lowered vitamin B6 rates in the body. Individuals with this type are likely to require more vitamin B6 levels.
Compensate by eating vitamin B6 rich foods, consume oral B group supplements and choose fortified foods. Around 89% Africans, 52% Caucasians, and 44% Asians carry this type of gene.
The MTR gene is responsible for converting folate into sources usable by the body.
A particular type of the gene is said to result in reduced MTR activity and causes a 30% increase in the risk of developing colorectal cancer. These individuals are likely to require more vitamin B6 levels (about twice more than the DRI values) to bring down the risk.
Oral supplements help match increased B6 needs. Fortified foods also make a difference.
Around 31% of Africans, 17% Caucasians, and 13% Asians carry this type of gene.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1265394/?page=1
https://pubmed.ncbi.nlm.nih.gov/23183295/
https://www.acs.org/content/acs/en/education/whatischemistry/landmarks/vitamin-b-complex.html
https://ods.od.nih.gov/factsheets/VitaminB6-HealthProfessional/
https://www.massgeneral.org/children/autism/lurie-center/vitamin-b6
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6357176/
https://www.sciencedirect.com/topics/biochemistry-genetics-and-molecular-biology/alpl
Folate, also known as vitamin B9, is a water-soluble B vitamin. It is naturally found in many folate-containing foods like spinach, broccoli, avocados, and lentils.
Apart from natural sources, the synthetic form of folate, folic acid, is also sold as a supplement. This form is supposedly absorbed better by the body.
Lucy Wills, a researcher, was the first one to identify folate and its function, in 1931. She demonstrated that anemia in pregnant women could be prevented/reversed with brewer's yeast. In the late 1930s, folate was isolated from brewer's yeast.
It was first extracted from spinach in 1941 - the term "folic" is from the Latin word 'Folium', which means leaf.
Further, the crystalline form of folate was extracted in 1943, which was the basis of the synthesis of Aminopterin, a derivative of folic acid.
Aminopterin was the first-ever anticancer drug developed, and its clinical efficacy was proved in 1948.
Vitamin D and folate are linked by their disparate sensitivities to Ultra Violet Radiation (UVR). While UVR stimulates the production of Vitamin D in the skin, it degrades folate through oxidation.
The hypothesis suggests that skin pigmentation may have evolved to maintain a balance in the levels of these vitamins.
The increased pigmentation observed in high-UVR regions was attributed to the need for protecting folate levels, while the depigmentation is low-UVR regions was a result of facilitating adequate vitamin D levels.
The VDR gene provides instructions for making a protein called Vitamin D Receptor, which allows the body to take in vitamin D. The different variants of the VDR genes are present in different frequencies across populations.
For example, the common VDR variant Fok1 has a lower frequency in African populations compared to European/Asian populations, while the frequency of another variant, Cdx2, is highest in African populations and the lowest in Europeans.
The difference in the frequency of these alleles across different ethnic populations can be attributed to the different UV regimes.
Several relationships are reported between UVR and folate metabolism genes. Two main enzymes involved in folate metabolism, serine hydroxymethyltransferase (SHMT) and methylenetetrahydrofolate reductase (MTHFR), have been studied to be UVR responsive.
For example, in regions where there’s a higher exposure to UVR, the frequency of a thermolabile MTHFR variant, C677T, is less.
These findings collectively provide strong molecular support to the Vitamin D-Folate hypothesis and showcase the existence of interactions between UVR, skin type, and vitamin D and folate genes.
Typically, the body has around 10-30 mg of folic acid stored in the liver, and 5-15 ng/mL in the blood.
In order to understand the recommended dosage of folic acid, the following terms are important:
It is important to note that the bioavailability of folate depends on the source. Synthetic vitamin B9 (folic acid) is readily absorbed (about 85%) into the body, compared to folate from food sources (about 50%). Dietary Folate Equivalent (DFE) was developed to reflect the total amount of bioavailable folic acid.
1 mcg DFE = 1 mcg food folate = 0.6 mcg of fortified foods/supplements taken with foods = 0.5 mcg folic acid in the form of a supplement (taken on an empty stomach).
A healthy adult needs 400mcg DFE folate daily. Pregnant women need 600 mcg of folate per day to meet the requirements of the growing fetus as well.
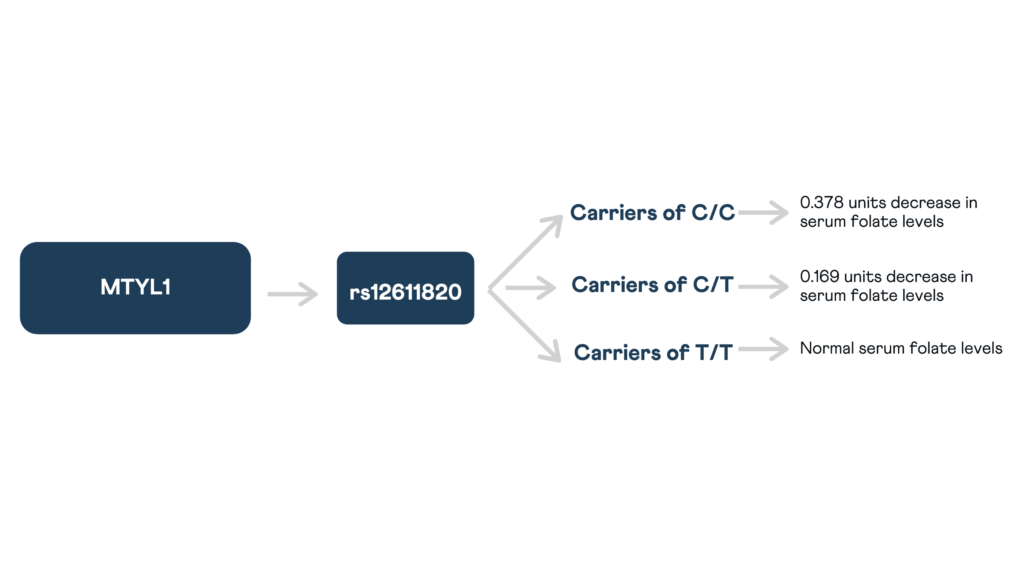
MTYL1 gene is located on chromosome 2.
It codes for myelin transcription factor 1, which is expressed in the neuronal tissues.
This transcription factor converts postnatal human fibroblasts into induced neuronal cells, thus playing a big role in cognitive function.
A variant in this gene is linked with serum folate levels.
This gives an initial idea of an association between folate levels and depression and schizophrenia.
rs12611820
A variation in this gene, with a C genotype, is reported to be linked to serum folate levels. In a GWAS study conducted, a single copy of the C allele was seen to decrease the serum folate levels by 0.169 units.
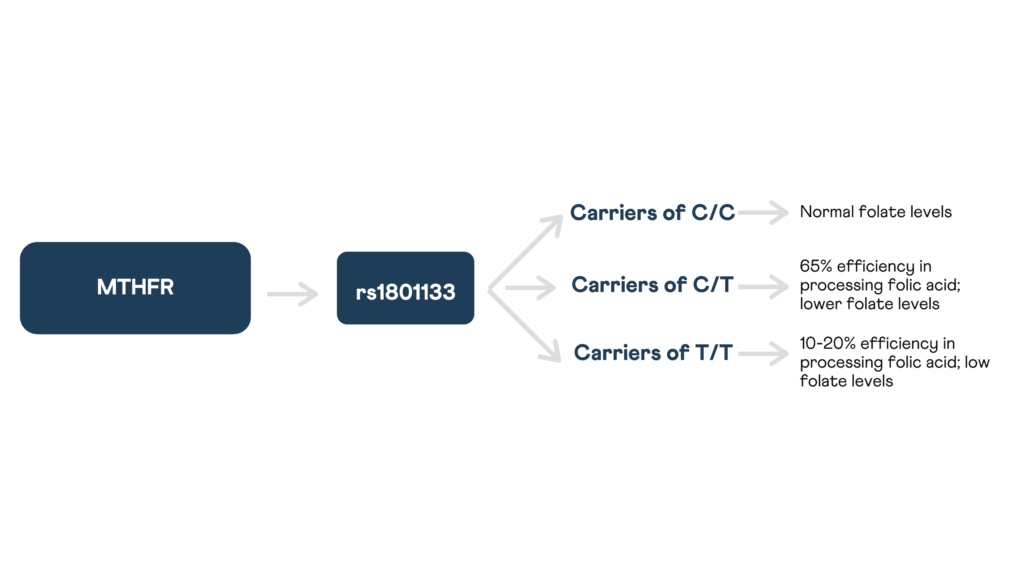
The MTHFR gene is located on chromosome 1. It codes for an enzyme called methylenetetrahydrofolate reductase, which plays a role in processing amino acids. This enzyme is involved in a chemical reaction that processes folate to its primary form (5-methyl tetrahydrofolate) found in the blood.
This compound is necessary for the multistep process that converts homocysteine to methionine.
In the normal functioning of the body, there is a balance between homocysteine and folate levels. However, when this balance is disturbed, it leads to health effects.
Mutations in the MTHFR gene have been associated with high homocysteine and low folate levels, both of which are harmful to the body.
rs1801133The most-studied variant of the MTHFR gene is 677T←C (rs1801133) in exon 5. The 677T variant has been studied to be less effective in the conversion of 5,10-methylenetetrahydrofolate to 5-methyltetrahydrofolate.
Thus, the serum folate concentration is lower in individuals with the 677TT genotype than in those with 677CC or 677CT genotypes.
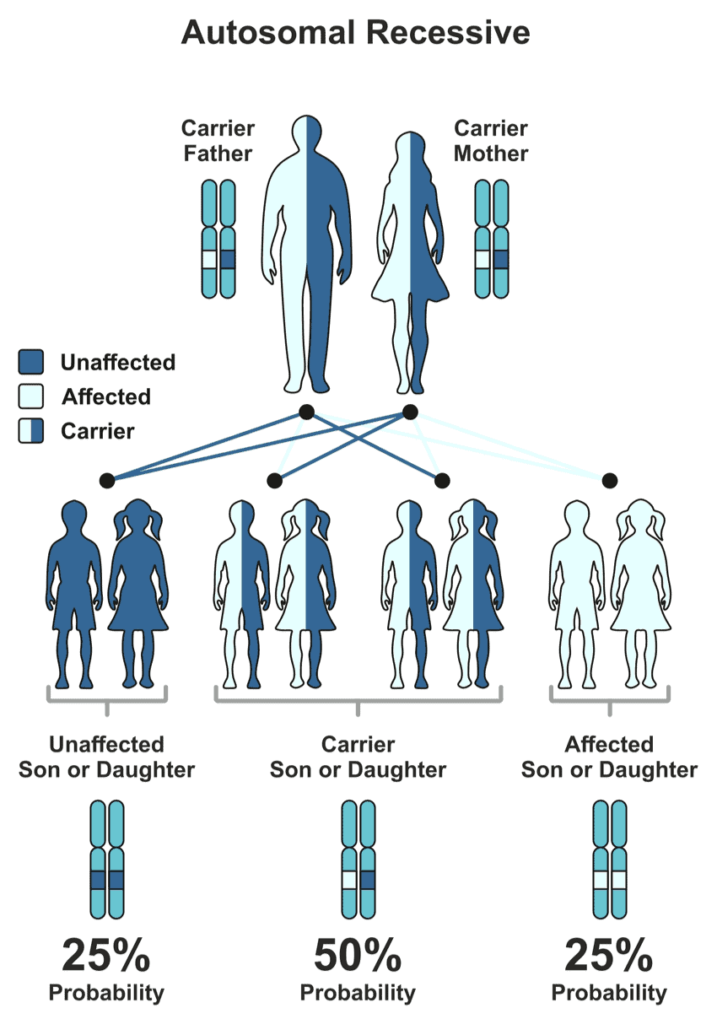
Inherited folate deficiency, also called Hereditary folate malabsorption, is a disorder that interferes with the body’s ability to absorb folates from food. Infants with this condition have normal folate levels at birth; however, they begin to show signs of folate deficiency within the first few months of life. Feeding difficulties, diarrhea, and failure to thrive are common signs observed in infants with inherited folate deficiency.
This condition is inherited in an autosomal recessive manner.
Now, for the expression of a recessive trait, both parents must pass on their recessive versions of traits.
A random process selects the gene to be passed down to the next generation.
In the case of autosomal recessive conditions, there is a 25% chance of occurrence.
If just one parent passes it on, the child will remain healthy but acts as a carrier of the gene.
Carriers could potentially pass it on to the coming generations.
Folate deficiency is usually a result of poor diet, alcoholism, and malabsorptive disorders. Hence the prevalence of isolated folate deficiency is pretty rare; other nutritional deficiencies mostly accompany it.
What Are The Signs And Symptoms Of Folate Deficiency
Causes of folate deficiency
Who’s at risk for folate inadequacy
It is rare to reach a toxicity level from consuming folate via natural food sources. An arbitrary upper limit for folic acid on a daily basis is 1000mcg.
Dangers of folate toxicity
Since vitamin B9 is water-soluble, it needs to be replenished in the body on a daily basis. There are a lot of sources of vitamin B9.
Folate is also available in the form of dietary supplements. Multivitamin supplements and B-complex tablets usually contain folic acid. These supplements are advised for individuals that have a mutation in the MTHFR gene.
It is recommended to take the active form of folic acid (L-methyl folate, or 5-MTHF). It is beneficial to have folic acid supplements daily to ensure optimal nutrient health for an individual.
Folate is an important vitamin that helps in cell replication, production of RBCs, and the maintenance of healthy cells in the body.
It is a water-soluble vitamin and should be included in the daily diet for a healthy individual.
There are vast implications if an individual has folate deficiency, with symptoms ranging from mouth sores to life-threatening anemia.
Pregnant women should also be wary of the amount of folic acid in their diet, as it can heavily impact the health of the fetus.
An individual can have inadequate folic levels because of an unbalanced diet, genetic variations, or other risk factors.
Folate deficient individuals can meet their requirements by adjusting their diet or taking supplements. When it comes to supplements, the dosage is an important factor.
Excess folate consumption can lead to folate toxicity the could result in a decline in cognition.
Thus, as always, it is recommended to consult a physician before starting any supplementation.
Vitamin B12 is one among the B vitamins and is also known as Cobalamin, since it contains the mineral called cobalt. This water-soluble vitamin cannot be made in the body and needs to be obtained from the food we eat.
Vitamin B12 helps with the below functions in the body:
Vitamin B12 deficiency can cause irreversible damage to the body and is, unfortunately, an increasing problem in the countries around the world. There are several reasons why your body might be receiving less vitamin B12 than the recommended daily intake. We will talk about that in the coming sections.
The story behind vitamin B12 goes as far back as the 1850s and includes the efforts of many renowned pathologists, physicists, and scientists.
Thomas Addison was an English physicist working in the famous Guy’s Hospital in London. Addison was working on the different causes and effects of diseases and identified a condition called Pernicious anemia.
Pernicious anemia is characterized by abnormal and insufficient Red Blood Cells. This disease was considered fatal between the 1800s and early 1900s.
It took almost 40 years to find a cure for pernicious anemia. George Hoyt Whipple, an American pathologist, had intensely analyzed the effects of food on the disease and concluded that a liver-based diet in dogs helped increase RBC count in the blood. This led to the identification of liver as a food-based treatment option for treating Pernicious anemia.
While doctors knew this diet helped reverse the condition, they didn’t fully understand why.
It took another 30 years for scientists to successfully identify and remove a water-soluble compound from liver samples and confirm that this was what actually treated the anemia. This compound’s structure was defined in 1956 and was named ‘vitamin B12’.
There were a total of five Nobel Prizes awarded to scientists around the world for the studies related to vitamin B12. We have these great minds to thank for bringing to the world’s notice one of the most important B vitamins.
Once you consume foods rich in Vitamin B12, gastric juices in the intestine help release the vitamin from the food. Once the vitamin is free, a particular protein called R-binder attaches itself to B12 and prevents the acids in the stomach from destroying the vitamin B12 molecule.
Now, the R-binder protein takes B12 to its next destination, the intrinsic factor (IF). This is also a kind of protein produced in the stomach.
From here, the B12 reaches an important carrier protein called Transcobalamin II. This helps circulate B12 to different parts of the body.
For the proper absorption and circulation of vitamin B12, the gastrointestinal tract and its help are vital. This is why people with gastric issues may have problems absorbing B12.
Did you know that your body stores enough quantities of vitamin B12 for future use? If you have been getting enough or more than the daily recommended values of vitamin B12, a certain amount keeps getting stored in the liver. This reserve can last for anywhere between 3 and 5 years!
The body knows the importance of vitamin B12 and hence keeps a stock of it for your benefit.
If you have been consistently getting lesser vitamin B12 than what’s needed, your excess reserve is continuously used and you start getting signs of vitamin B12 deficiency only after a couple of years.
The rate at which the stored levels are depleted (turnover rate) depends on your body’s ability to get and absorb vitamin B12. Healthy individuals with normal absorption rates may have a lesser turnover rate than those with gastrointestinal issues or pernicious anemia.
The Dietary Reference Intake (DRI) is a reference for assessing the general needs of vitamin B12 levels in children and adults on an everyday basis.
Excess of vitamin B12 does not cause toxicity in the body as fat-soluble vitamins do.
Vitamin B12 that is ingested is used for everyday functioning and a part of it keeps getting stored in the liver as a reserve. The remaining doses are easily excreted out through urine. Hence it is not very easy to get an overdose when it comes to B12.
However, if you are on vitamin B12 shots, supplements, and a diet rich in red meat, poultry, and dairy products simultaneously, excess quantities of the vitamin may cause dizziness, nausea, and headaches in some individuals.
When you are consuming lesser vitamin B12 than the DRI values, you are at risk of developing the below conditions.
The FUT2 gene encodes a protein that helps a harmful bacteria called Helicobacter pylori attach itself to the digestive tract. This bacteria can inhibit the absorption of vitamin B12 in the body. Here is a list of FUT2 gene variants that can result in increased/ decreased levels of vitamin B12 in the body.
The TCN2 gene encodes a protein that helps in the final transportation of vitamin B12 from the blood to the cells in the body. A certain variant of the TCN2 gene in the Caucasian population is known to cause increased/decreased levels of B12 in the body.
Maintaining healthy vitamin B12 levels in the body is beneficial for overall health maintenance. It keeps you energetic, strong, and healthy. Here are expert recommendations on getting your daily dose of vitamin B12 right.
https://www.animalresearch.info/en/medical-advances/timeline/pernicious-anaemia/
https://ods.od.nih.gov/factsheets/VitaminB12-Consumer/
https://ods.od.nih.gov/factsheets/VitaminB12-HealthProfessional/
https://www.ncbi.nlm.nih.gov/books/NBK114329/ https://www.sciencedirect.com/topics/agricultural-and-biological-sciences/vitamin-b12
